Introduction
Watching your senior dog struggle to stand up, hesitate before climbing stairs, or limp after a short walk is heartbreaking. For millions of dog owners, hip dysplasia and the osteoarthritis it causes represent one of the most common and debilitating challenges of canine aging. Large breeds like Labrador Retrievers, Golden Retrievers, and German Shepherds are especially vulnerable, but hip dysplasia can affect dogs of all sizes. While surgery remains an option for severely affected dogs, many owners seek effective, non-invasive alternatives. Extracorporeal shockwave therapy (ESWT) offers a drug-sparing, non-surgical solution that reduces pain, improves mobility, and helps senior dogs return to the active, joyful lives they deserve.
1. Understanding Hip Dysplasia and Canine Osteoarthritis
1.1 What Is Hip Dysplasia?
Hip dysplasia is a multifactorial developmental abnormality of the coxofemoral (hip) joint in dogs, characterized by joint laxity and subsequent degenerative joint disease and osteoarthritis. Excessive and rapid growth, exercise, nutrition, and hereditary factors all influence the occurrence of hip dysplasia. The condition is most common in large-breed dogs, but it also affects small-breed dogs and cats. The pathophysiological basis is a disparity between hip joint muscle mass and rapid bone development, which leads to coxofemoral joint laxity and instability.
1.2 The Progression to Osteoarthritis
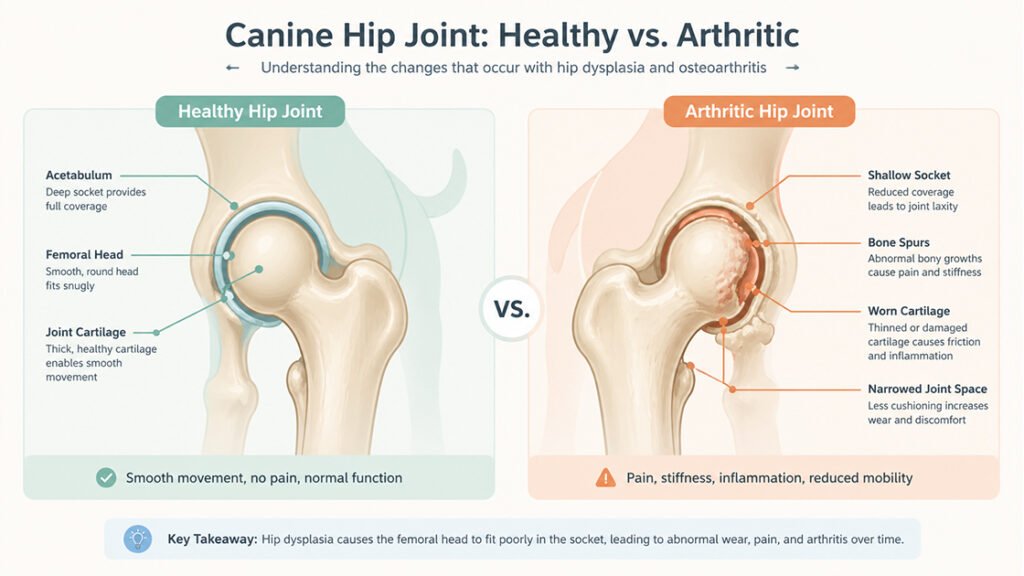
Once joint laxity develops, the femoral head no longer fits snugly in the acetabulum (hip socket). This abnormal movement causes excessive wear on the joint cartilage, leading to secondary osteoarthritis. Degenerative changes include acetabular bone sclerosis, osteophytosis (bone spurs), thickened femoral neck, joint capsule fibrosis, and subluxation or luxation of the femoral head. The clinical signs of hip dysplasia vary and do not always correlate with radiographic abnormalities. Lameness can range from mild to severe and is often more pronounced after exercise or, once osteoarthritis has developed, shortly after rest. A bunny-hopping gait is sometimes evident, and dogs may show joint laxity (Ortolani sign), decreased range of motion, crepitus, and pain during full extension and flexion.
1.3 Why Senior Dogs Suffer Most
Osteoarthritis (OA) affects an estimated 20% of adult dogs and up to 80% of geriatric dogs, making it a leading cause of chronic pain, impaired mobility, and reduced quality of life. For senior dogs, the cumulative effects of years of abnormal joint mechanics—combined with age-related muscle loss (sarcopenia), weight gain, and reduced activity—create a cycle of declining function and increasing pain. Many owners consider euthanasia when their elderly dog can no longer get up or walk comfortably. This makes effective, accessible pain management for senior dogs not just a quality-of-life issue but a matter of life and death.
2. How Shockwave Therapy Works for Hip Pain
2.1 The Science of Acoustic Waves
Extracorporeal shockwave therapy delivers high-energy acoustic sound waves that penetrate deep into the body‘s tissues. Despite its name, ESWT has nothing to do with electrical shock. Instead, it uses focused, high-velocity sound waves that travel through your dog’s skin, subcutaneous tissue, fascia, and muscle to reach the affected hip joint and surrounding structures. As the waves pass through layers of tissue with different densities—such as the bone–tendon interface of the hip—they release stored energy that stimulates biological changes at the cellular level. When used appropriately, ESWT can result in decreased pain, decreased inflammation, and improved healing of both bone and soft tissue.
2.2 Focused vs. Radial Technology: Why Depth Matters
Not all shockwave devices are created equal for treating deep hip joints. Focused extracorporeal shockwave therapy (ESWT) offers adjustable penetration depth (5–40mm or more) for anatomical precision, making it ideal for targeting the deep structures of the coxofemoral joint. Focused technology uses a targeted wave pattern for specific tissue planes, and over 90% of patients tolerate awake treatment with minimal discomfort. In contrast, radial pressure wave therapy has significant limitations for deep hip pathology: it cannot target specific tissue depths, its energy is strongest at the skin surface with a diverging pattern, and it is often louder and more painful for patients. For senior dogs with deep-seated hip pain, focused ESWT is the superior choice.
2.3 Biological Responses to Shockwave Therapy
Research in both experimental models and clinical settings has demonstrated multiple beneficial biological responses to ESWT:
- Neovascularization: Shockwaves stimulate new blood vessel growth, improving tissue oxygenation and nutrient delivery to the arthritic hip joint.
- Cartilage preservation: Reduced nitric oxide production and inhibition of chondrocyte apoptosis help protect cartilage from further degenerative changes.
- Bone remodeling: ESWT enhances osteoblastic activity (new bone formation) while stimulating osteoclastic activity to remodel bone spurs and mineralized deposits.
- Analgesic effects: Depletion of substance P and modulation of nociceptors contribute to reduced pain perception.
- Mechanotransduction: Physical microstress in tissues triggers molecular signaling pathways, releasing cytokines such as TGF-β1 and VEGF, which further support healing.
In osteoarthritis specifically, ESWT primarily provides symptomatic pain relief, though it does not halt or reverse disease progression. For senior dogs with hip dysplasia, this pain relief translates directly into improved mobility and quality of life.
3. Core Mechanisms of Shockwave Therapy for Canine Hip Dysplasia
3.1 Stimulating Neovascularization in Arthritic Joints
Chronic hip osteoarthritis leads to reduced blood flow to the joint capsule and surrounding tissues, limiting the delivery of oxygen and nutrients needed for repair. Shockwave therapy generates high‑energy acoustic waves that penetrate deep into the coxofemoral joint. These waves trigger the release of angiogenic factors, including vascular endothelial growth factor (VEGF). The result is the formation of new capillaries (neovascularization) within the joint capsule, synovial membrane, and subchondral bone. Improved microcirculation brings fresh oxygen, glucose, and growth factors to the damaged cartilage and bone, supporting tissue repair and reducing the ischemic stress that contributes to pain.
3.2 Reducing Inflammatory Mediators and Pain Signaling
Osteoarthritis involves a chronic low‑grade inflammatory state driven by pro‑inflammatory cytokines such as IL‑1β, IL‑6, and TNF‑α. These molecules sensitize nociceptors, amplify pain signals, and accelerate cartilage degradation. Shockwave therapy modulates this inflammatory cascade by reducing the production of these cytokines while increasing anti‑inflammatory mediators. The treatment also depletes substance P from peripheral nerve endings and downregulates pain‑transmitting receptors. This dual effect—less inflammation and reduced pain signaling—provides natural, drug‑free relief without the side effects of oral anti‑inflammatories.
3.3 Promoting Cartilage Preservation and Subchondral Bone Remodeling
The mechanical forces generated by shockwaves directly affect chondrocytes (cartilage cells) and osteocytes (bone cells). In the arthritic hip, excessive nitric oxide production leads to chondrocyte apoptosis (cell death) and matrix degradation. Shockwave therapy suppresses nitric oxide synthase activity, protecting chondrocytes from oxidative damage. At the same time, focused acoustic waves stimulate osteoblasts to remodel subchondral bone, reducing the formation of painful bone spurs (osteophytes) and improving the congruence between the femoral head and acetabulum. This process helps slow the progression of joint degeneration.
3.4 Mechanotransduction and Endogenous Healing Activation
Living tissues respond to mechanical forces through a process called mechanotransduction. The high‑velocity sound waves of ESWT act as a physical signal that cells interpret as a “need to repair.” This signal activates integrins on cell surfaces, which in turn trigger intracellular pathways involving focal adhesion kinase (FAK) and extracellular signal‑regulated kinase (ERK). These pathways upregulate the expression of growth factors such as transforming growth factor‑beta (TGF‑β1) and insulin‑like growth factor (IGF‑1). The result is a coordinated healing response that includes collagen synthesis, matrix reorganization, and recruitment of progenitor cells to the damaged joint.
4. The Treatment Process: What to Expect
4.1 Initial Evaluation and Preparation
Before any shockwave treatment, your veterinarian will perform a thorough orthopedic examination, which may include radiographs to assess the extent of hip dysplasia and osteoarthritis. Not all dogs are ideal candidates for ESWT. The treatment should NOT be used in dogs with immune-mediated joint disease, infected joints, infected intervertebral discs (discospondylitis), or dogs that are still actively growing. For senior dogs with stable, chronic hip osteoarthritis, ESWT is generally safe and appropriate.
4.2 During the Session
A typical ESWT session for canine hip dysplasia takes only 3 to 5 minutes per treatment area. Your dog will lie comfortably on a padded surface while the veterinarian applies the handheld probe (called a trode) to the skin over the hip joint. Generous coupling gel ensures proper transmission of the sound waves into the tissue. Fur over the treatment area is usually clipped short because fur can create air pockets between the trode and the skin, reducing the amount of energy delivered to the target tissue.
Most dogs tolerate focused ESWT well while awake. In fact, many dogs even become more relaxed during the treatment. The sensation is not painful—patients typically indicate through subtle movement or vocalization exactly where the energy is needed, allowing the practitioner to target the precise location of pain. With modern equipment, sedation is rarely necessary for routine osteoarthritis cases.
4.3 Treatment Frequency and Duration
ESWT is typically delivered as a series of treatments, not a single session. Most protocols recommend 3 to 6 treatments spaced 2 to 3 weeks apart. The number and frequency vary depending on the device used, the severity of the condition, and your dog‘s individual response. A standard osteoarthritis protocol often involves 3 treatments at weekly intervals, followed by reassessment. Many dogs show improvement after the first treatment, but the full benefit usually accumulates over the course of the series. Some dogs require maintenance sessions every 2 to 4 weeks or as needed to sustain pain relief and mobility gains.
4.4 Post-Treatment Care and Expectations
Because shockwave therapy provides potent analgesic effects for the first 48 hours after treatment, rest is recommended to prevent any further damage to the tissues. Additionally, because of the mechanism of action, the use of anti-inflammatory medications and/or cryotherapy around shock wave treatment times should be avoided. You may notice your dog moving more comfortably within hours of the first session. However, optimal results often take several weeks to fully manifest as the biological healing processes—neovascularization, tissue remodeling, and pain modulation—run their course.
5. Integrating Shockwave Therapy into a Comprehensive Senior Dog Care Plan
5.1 A Multimodal Approach to Hip Dysplasia
Shockwave therapy works best as part of a multimodal management plan, not as a stand-alone treatment. For many dogs with mild to moderate hip dysplasia, non-surgical options can help reduce pain and improve quality of life. These options include weight control (reducing body weight significantly decreases joint loading), physical therapy and hydrotherapy to build muscle mass without stressing the hips, and joint supplements containing omega-3 fatty acids, glucosamine, and chondroitin. Weight management is particularly critical: a landmark study of 70 dogs with hip osteoarthritis found that a therapeutic diet significantly reduced synovitis (joint inflammation), increased flexion and extension of the coxofemoral joint, and notably decreased pain.
5.2 When Shockwave Therapy Works Best
Shockwave therapy works best for dogs with stable, chronic hip osteoarthritis that has not responded adequately to conservative care. When hip dysplasia is mild and clinical signs are minimal, weight management and controlled exercise alone may be sufficient. In cases of moderate to severe pain, limping, and mobility limitations—particularly for dogs that cannot tolerate long-term NSAID use due to liver or kidney concerns—shockwave therapy provides a valuable drug‑sparing alternative. After surgical procedures such as total hip replacement or femoral head ostectomy (FHO), ESWT can also support post‑surgical rehabilitation by reducing pain and inflammation and accelerating return to function.
5.3 Monitoring Progress
Tracking your dog‘s response to treatment helps your veterinarian adjust the protocol as needed. Keep a simple log of observations: How easily does your dog rise from lying down? How far can they walk before limping? Do they climb stairs willingly or hesitate? Are they playing more? Many clinics use validated outcome measures like the Canine Brief Pain Inventory (CBPI) or the Liverpool Osteoarthritis in Dogs (LOAD) questionnaire to objectively assess changes in pain and function. These tools help document improvement and guide decisions about maintenance therapy.
5.4 Long-Term Maintenance for Senior Dogs
Osteoarthritis is a progressive, chronic condition. Even after a successful course of shockwave therapy, many senior dogs benefit from ongoing maintenance. Some owners schedule a shockwave session every 2 to 4 weeks or whenever they notice their dog‘s mobility beginning to decline again. This proactive approach keeps pain at bay, reduces reliance on daily medications, and maintains your senior dog’s quality of life over the long term. Many geriatric dogs have been able to remain comfortable and active for years with regular maintenance shockwave therapy, avoiding the euthanasia that owners feared was inevitable.
6. Safety, Cautions, and When to Seek Veterinary Care
6.1 Who Should Not Receive ESWT
While shockwave therapy is very safe for the vast majority of senior dogs, certain conditions warrant exclusion. ESWT should NOT be used in dogs with immune-mediated joint disease, infected joints, infected intervertebral discs (discospondylitis), or dogs that are still actively growing. Dogs with bleeding disorders or those taking anticoagulant medications should be evaluated carefully. Pregnant or lactating dogs should not receive ESWT. Additionally, ESWT should never be applied directly over the eyes, major nerves, the spinal cord, or the abdomen during pregnancy.
6.2 What to Watch For After Treatment
Most dogs experience no adverse effects from ESWT. Some may show mild, temporary soreness or sensitivity in the treated area for 24 to 48 hours after the session. This is normal and indicates that the biological healing response has been activated. If you notice worsening lameness, significant swelling, or signs of systemic illness, contact your veterinarian promptly. Because ESWT provides potent pain relief, it is essential to rest your dog for the first 48 hours after treatment to prevent overactivity that could mask pain and cause further injury.
6.3 The Importance of Veterinary Oversight
Shockwave therapy should always be administered by a licensed veterinarian or certified veterinary rehabilitation therapist. Proper patient selection, correct device settings, and accurate anatomical targeting are essential for both safety and efficacy. Never attempt to use human shockwave devices on your dog, and do not rely on unproven home devices. A professional veterinary rehabilitation evaluation ensures that shockwave therapy is appropriate for your dog’s specific condition and that it is integrated correctly with other treatments.
FAQ
Q: How many shockwave sessions will my senior dog need for hip dysplasia?
A: Most dogs require 3 to 6 sessions spaced 2 to 3 weeks apart. Some dogs show improvement after 1 session, while others need the full series to achieve optimal results.
Q: Does shockwave therapy hurt my dog?
A: No. Most dogs tolerate the treatment comfortably while awake. The sensation is not painful, and many dogs even relax or fall asleep during the session.
Q: Will shockwave therapy cure my dog‘s hip dysplasia?
A: No. Shockwave therapy provides pain relief and improves mobility but does not cure the underlying structural abnormality of hip dysplasia. However, for many senior dogs, this pain relief is enough to restore quality of life.
Q: Can shockwave therapy replace my dog‘s arthritis medications?
A: For some dogs, shockwave therapy significantly reduces or eliminates the need for daily NSAIDs. Your veterinarian will help determine whether medication reduction is appropriate based on your dog‘s response.
Q: Is shockwave therapy covered by pet insurance?
A: Coverage varies by insurance provider and plan. Many pet insurance plans cover shockwave therapy when prescribed by a veterinarian for osteoarthritis or other orthopedic conditions. Check with your provider for specific coverage details.
Conclusion
For senior dogs suffering from hip dysplasia and osteoarthritis, every step can be a struggle. The pain of climbing stairs, rising from a nap, or simply walking across the room steals their joy and erodes their quality of life. Extracorporeal shockwave therapy offers a non-invasive, drug-sparing solution that works at the cellular level to reduce inflammation, stimulate healing, and restore pain-free mobility. By stimulating neovascularization, reducing inflammatory mediators, protecting cartilage, and activating endogenous healing pathways, shockwave therapy helps senior dogs regain comfort and function. When integrated with weight management, physical rehabilitation, and appropriate nutrition, shockwave therapy can help your senior dog go from limping to leaping—and enjoy their golden years to the fullest.
References
Boström, A., et al. (2022). Systematic Review of Complementary and Alternative Veterinary Medicine in Sport and Companion Animals: Extracorporeal Shockwave Therapy. Animals (Basel).
https://pubmed.ncbi.nlm.nih.gov/36428352/
PulseVet. (2025). Shock Wave & PEMF Therapy for Dogs: Evidence-Based Rehabilitation Protocols.
https://pulsevet.zomedica.com/shock-wave-pemf-therapy-dogs-veterinary-rehabilitation/
PulseVet. (2025). When Your Dog is Limping: A Non-Invasive Solution That Could Change Everything.
https://pulsevet.zomedica.com/dog-limping-shock-wave-therapy-solution/
Skalicky, M., et al. (2007). Effects of radial shockwave therapy on the limb function of dogs with hip osteoarthritis. The Veterinary Record.
https://www.researchgate.net/publication/6290219
Shockwave Canada. Shockwave Therapy for Dogs – Treating Hip Dysplasia.
https://shockwavecanada.com/shockwave-therapy-for-dogs-treating-hip-dysplasia/
IVC Journal. (2026). When sound becomes medicine: shockwave therapy for canine osteoarthritis.
https://ivcjournal.com/when-sound-becomes-medicine-shockwave-therapy-in-canine-arthritis-care/
VCA Animal Hospitals. Extracorporeal Shockwave Therapy.
https://vcahospitals.com/know-your-pet/extracorporeal-shockwave-therapy
Horne, C. R., & Schnabel, L. V. (2025). Extracorporeal shock wave therapy in equine and canine practice. Journal of the American Veterinary Medical Association.
https://avmajournals.avma.org/view/journals/javma/aop/javma.25.12.0827/javma.25.12.0827.xml
Healing Paws Center. (2025). Shockwave Therapy for Dogs & Cats.
https://healingpawsfl.com/shockwave-therapy-for-dogs-cats-in-oakland-park/
Merck Veterinary Manual. (2025). Hip Dysplasia in Dogs.
