Introduction
Myofascial trigger points are a frequent yet often overlooked source of musculoskeletal pain, affecting office workers, athletes, manual laborers, and individuals with repetitive strain patterns. These hypersensitive nodules within muscle tissue can cause localized discomfort, referred pain, stiffness, and reduced mobility that interfere with daily function and quality of life. While conventional approaches such as massage, manual therapy, and dry needling are widely used, many patients experience only partial or short-term relief. Shockwave therapy—commonly referred to as extracorporeal shock wave therapy (ESWT)—has gained growing attention as a non-invasive option for managing myofascial pain. By delivering acoustic energy into affected soft tissues, this modality may help reduce muscle tension, support circulation, and modulate pain sensitivity. In modern rehabilitation settings, shockwave therapy is increasingly integrated into comprehensive care plans for patients with persistent muscle knots. This clinical guide explores how the therapy works, who may benefit most, and how it fits into contemporary musculoskeletal management.
1. Understanding Myofascial Trigger Points
Before discussing treatment strategies, it is important to understand what trigger points are and why they can be so persistent.
1.1 What Are Myofascial Trigger Points?
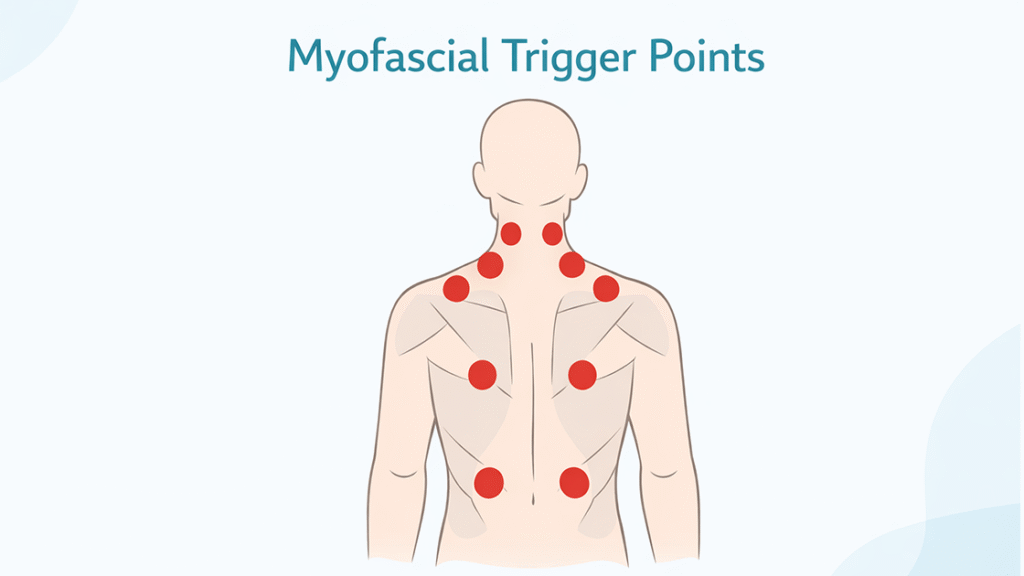
Myofascial trigger points are hyperirritable spots located within taut bands of skeletal muscle. Clinicians often identify them through palpation, where they feel like small, firm nodules embedded in tight muscle fibers. When pressure is applied, these points may produce local tenderness and sometimes referred pain that travels to other regions of the body.
Trigger points are typically categorized as either active or latent. Active trigger points produce spontaneous pain and are often responsible for a patient’s primary complaint. Latent trigger points may not cause continuous discomfort but can still restrict movement and contribute to muscle dysfunction. Both types can interfere with normal biomechanics, especially when multiple trigger points develop within the same muscle group.
From a functional standpoint, trigger points contribute to reduced muscle elasticity, altered movement patterns, and protective guarding. Over time, this can lead to compensatory strain in surrounding tissues, perpetuating a cycle of discomfort and limited mobility.
1.2 Common Causes of Myofascial Pain
The development of trigger points is usually multifactorial. Repetitive muscle overload is one of the most common contributors, particularly in individuals who perform the same movement patterns for extended periods. Office workers who spend long hours at a computer, for example, frequently develop trigger points in the upper trapezius and levator scapulae due to sustained postural stress.
Poor ergonomics and forward head posture are also significant risk factors. When muscles are held in shortened or strained positions for prolonged periods, localized metabolic stress can occur, contributing to trigger point formation. Athletes may develop trigger points following acute muscle strain, overtraining, or inadequate recovery between workouts.
Psychological stress can play a role as well. Increased muscle tension associated with stress responses may predispose certain individuals to chronic muscle tightness. Additionally, biomechanical imbalances—such as hip instability or altered gait mechanics—can overload specific muscle groups and promote trigger point development.
Because these contributing factors often coexist, effective management typically requires a multimodal approach rather than reliance on a single intervention.
2. Why Treat Trigger Points with Shockwave Therapy?
As rehabilitation professionals seek more efficient and durable solutions for myofascial pain, shockwave therapy has become an increasingly popular adjunct.
2.1 Limitations of Traditional Approaches
Conventional trigger point treatments remain valuable, but they are not without challenges. Manual therapy techniques, including ischemic compression and soft tissue mobilization, often depend heavily on practitioner skill and may require frequent sessions to maintain results. Some patients experience only temporary relief before muscle tension returns.
Dry needling can be effective for certain individuals, yet it is invasive and not universally tolerated. Patients with needle sensitivity or anxiety may avoid this option altogether. Massage therapy, while helpful for relaxation and circulation, may not always reach deeper or more stubborn trigger points.
Injection-based approaches are typically reserved for more persistent cases but involve greater complexity and patient apprehension. Collectively, these limitations have encouraged clinicians to explore complementary, non-invasive modalities that can be delivered consistently and efficiently.
2.2 How Shockwave Therapy Affects Muscle Knots
Shockwave therapy works by transmitting mechanical acoustic energy into targeted soft tissue. Unlike surface-level treatments, the energy waves propagate through the skin and into underlying muscle structures, where they create controlled mechanical stimulation.
This stimulation is believed to influence trigger points in several helpful ways. First, it may help reduce excessive muscle tone by mechanically interacting with contracted muscle fibers. Many clinicians observe that treated areas often feel less rigid following therapy, suggesting a reduction in localized hypertonicity.
Second, shockwave therapy may support microcirculatory changes in the treated region. Improved local blood flow can enhance oxygen delivery and facilitate the removal of metabolic byproducts that accumulate in chronically tight muscle tissue. This shift in the local tissue environment may contribute to reduced sensitivity and improved tissue quality.
Additionally, acoustic stimulation may influence nociceptor activity—the sensory receptors involved in pain perception. By modulating these signals, shockwave therapy may help decrease the heightened pain response often associated with trigger points.
Perhaps most importantly, the therapy may help interrupt the well-known pain-spasm-pain cycle. When muscle tightness leads to pain and pain leads to further guarding, trigger points can persist for months or even years. Mechanical stimulation from shockwave therapy may help break this cycle and support more normalized muscle function.
3. Clinical Benefits of ESWT for Myofascial Pain
When incorporated appropriately into patient care, shockwave therapy offers several practical advantages.
3.1 Key Therapeutic Advantages
One of the most appealing features of shockwave therapy is its non-invasive nature. Because the treatment does not require needles or incisions, it is generally well accepted by patients seeking conservative care options. Sessions are typically brief, making the modality easy to integrate into busy clinical schedules.
Another advantage is the ability to target deeper soft tissue structures that may be difficult to influence with superficial modalities alone. This is particularly relevant for larger muscle groups such as the gluteals or calf complex, where trigger points can be more resistant to manual techniques.
Recovery demands are minimal. Most patients can resume normal daily activities immediately after treatment, which is important for working adults and active individuals who cannot afford extended downtime. The therapy also pairs well with other rehabilitation strategies, allowing clinicians to build comprehensive treatment plans without significant scheduling conflicts.
3.2 Expected Functional Improvements
Patients undergoing shockwave therapy for myofascial trigger points often report gradual but meaningful improvements. Reduced localized tenderness is commonly noted as muscle sensitivity decreases. Many individuals also experience less referred pain, particularly in chronic neck and shoulder cases.
Improved tissue flexibility may translate into better range of motion and smoother movement patterns. For athletes and physically active patients, this can support more efficient training and reduced post-activity soreness. Office workers frequently report decreased muscle tightness and improved comfort during prolonged sitting.
It is important to recognize that response timelines vary. Chronic cases that have persisted for years may require a longer course of care compared with more recent muscle dysfunction. Nevertheless, when combined with appropriate corrective strategies, shockwave therapy can play a valuable role in functional recovery.
4. Clinical Application Considerations
Successful outcomes with shockwave therapy depend not only on the technology itself but also on thoughtful clinical implementation.
4.1 Importance of Thorough Assessment
Accurate identification of trigger points remains essential. Skilled palpation helps clinicians distinguish between true myofascial nodules and more generalized muscle tenderness. Functional assessment is equally important, as trigger points often develop secondary to movement dysfunction elsewhere in the kinetic chain.
Evaluating posture, joint mobility, and movement patterns can reveal contributing factors that must be addressed alongside local treatment. Without this broader perspective, trigger points may recur even after initially successful therapy.
Patient education also plays a key role. When individuals understand how posture, workload, or training habits contribute to muscle tension, they are more likely to adopt preventive strategies that support long-term results.
4.2 Technique and Patient Comfort
Although shockwave therapy is generally well tolerated, clinician attentiveness to patient feedback enhances the experience. Clear communication during treatment helps ensure that stimulation remains within a comfortable range.
Gradual progression and consistent contact with the treatment area typically improve tolerance. Many clinicians also find it helpful to reassess tissue response periodically throughout the care plan, adjusting their approach based on how the muscle responds over time.
5. Common Target Muscles for Shockwave Therapy
Certain muscle groups are particularly prone to clinically significant trigger points.
5.1 Upper Trapezius
The upper trapezius is one of the most frequently affected muscles, especially among office workers and individuals with prolonged screen time. Trigger points in this region often contribute to neck stiffness, shoulder tension, and tension-type headaches.
5.2 Levator Scapulae
This muscle is commonly involved in patients with forward head posture and cervical strain patterns. Individuals may report discomfort along the inner border of the shoulder blade and difficulty with neck rotation.
5.3 Gluteal Region
The gluteus medius and piriformis frequently develop trigger points in runners and patients with hip instability. Symptoms may include lateral hip pain or buttock discomfort that can mimic sciatic irritation.
5.4 Calf Muscles
Athletes and individuals who spend long hours standing often develop trigger points in the gastrocnemius and soleus complex. These can contribute to lower-limb fatigue, tightness, and reduced ankle mobility.
6. Integrating Shockwave into Multimodal Care
Shockwave therapy tends to be most effective when used as part of a comprehensive rehabilitation strategy.
6.1 Combination with Manual Therapy
Soft tissue mobilization and joint techniques may complement shockwave treatment by addressing surrounding tissue restrictions. Together, these approaches can support improved tissue extensibility and circulation.
6.2 Role of Corrective Exercise
Targeted exercise is critical for long-term success. Strengthening weak muscle groups and improving movement control helps reduce the mechanical overload that often drives trigger point formation in the first place.
6.3 Importance of Stretching and Mobility Work
Post-treatment stretching and mobility exercises help maintain gains in tissue flexibility. Regular home programs empower patients to participate actively in their recovery, which is strongly associated with better outcomes.
7. Safety Considerations
Shockwave therapy is generally well tolerated when applied appropriately. Some patients may experience mild temporary soreness or redness in the treated area, which typically resolves quickly. Proper screening remains important, and clinicians should evaluate each patient’s medical history and local tissue status before initiating care.
FAQ
Does shockwave therapy hurt muscle knots?
Most patients describe the sensation as tolerable and adjustable. Comfort levels can be modified during treatment.
How many sessions are usually needed?
Many patients undergo a short series of treatments, though chronic cases may require a longer course depending on individual response.
Is shockwave therapy better than dry needling?
Each modality has its role. Shockwave therapy offers a non-invasive alternative and is often used alongside other techniques.
When will improvement be noticeable?
Some patients notice early changes, while others experience gradual improvement over several weeks.
Can trigger points return?
Yes. Without addressing posture, workload, or movement mechanics, recurrence is possible.
Conclusion
Shockwave therapy has emerged as a valuable non-invasive tool for managing myofascial trigger points in modern rehabilitation practice. By mechanically stimulating affected tissues, supporting circulation, and modulating pain sensitivity, the therapy may help reduce muscle tension and improve functional movement. When combined with thorough assessment, corrective exercise, and patient education, shockwave therapy can play an important role in comprehensive myofascial pain management.
References
Extracorporeal Shock Wave Therapy in Musculoskeletal Disorders
https://www.ncbi.nlm.nih.gov/books/NBK482448
Myofascial Trigger Points: Pathophysiology and Treatment
https://www.sciencedirect.com/topics/medicine-and-dentistry/myofascial-trigger-point
Shockwave Therapy in Physical Medicine and Rehabilitation
